Breast Reduction and Insurance: How to Obtain Coverage
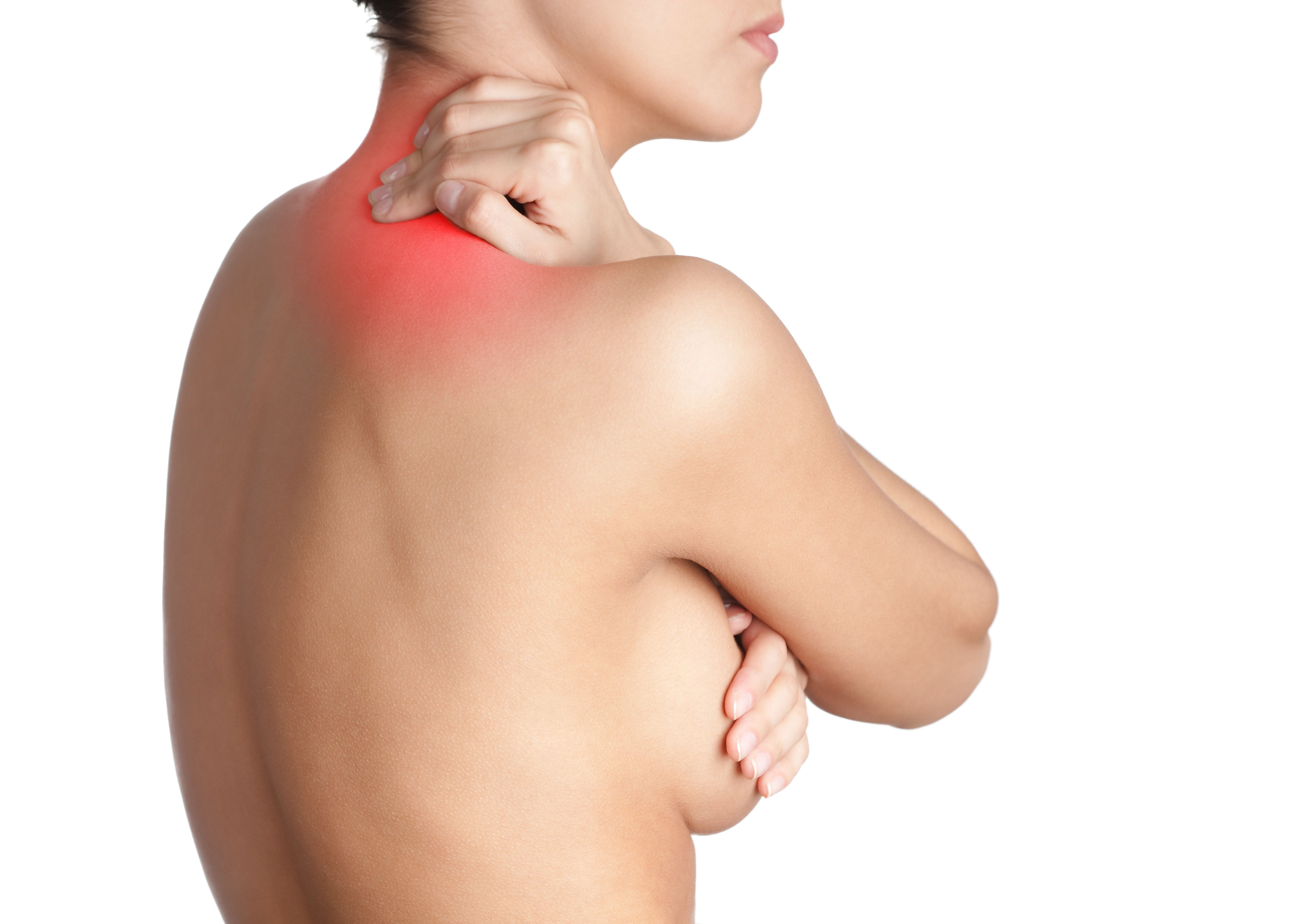 Women who suffer from macromastia, or enlarged breasts, can benefit from breast reduction at our Manhattan, NY cosmetic surgery practice. Breast reduction can alleviate symptoms of macromastia, including neck, back, and shoulder pain.
Women who suffer from macromastia, or enlarged breasts, can benefit from breast reduction at our Manhattan, NY cosmetic surgery practice. Breast reduction can alleviate symptoms of macromastia, including neck, back, and shoulder pain.
The problem, however, is that breast reduction is typically considered cosmetic unless there is documentation showing that the procedure is medically necessary.
Here, Dr. Oren Z. Lerman discusses breast reduction and insurance while providing insight on how to obtain appropriate coverage for your procedure.
Why Documentation Is Important
Health insurance offers many benefits. However, it can be frustrating for patients when insurance companies fail to cover a procedure. After all, it should be enough that a cosmetic surgeon recommends a breast reduction to alleviate symptoms of macromastia, right?
It should be. But it isn’t. Many patients are surprised to find out that most insurance carriers require additional documented reports from other specialists before they will consider covering the procedure. Furthermore, many of them require six to 12 months of non-surgical treatment as well.
What Does This Mean?
Essentially, if you are considering a breast reduction to reduce chronic pain, begin the preliminary process now. Schedule consultations with other medical professionals such as physical therapists, chiropractors, orthopedic surgeons, or dermatologists.
These professionals can evaluate your situation and give your insurance carrier specific reasons why a breast reduction procedure is in your best interests. The sooner you start gathering documentation, the sooner your procedure will be a reality.
Reasons Why Breast Reduction May Be Medically Necessary
It is important to understand that every insurance company (and representative, for that matter) is different. Therefore, each carrier will have their own unique set of criteria. In the sections below, we will briefly discuss the most common qualifications that can make patients eligible for breast reduction.
Chronic Pain
Do you experience back, neck, or shoulder pain? Do you commonly develop inflammation under the breasts? These symptoms can be legitimate cause for breast reduction.
Of course, these conditions must be routinely monitored by a physician, as they will mostly likely be required to submit letters to your insurance company.
No Success with Alternative Treatments
In some cases, it may be necessary to try a number of alternative treatments before being approved for breast reduction coverage. This may include things like weight loss, chiropractic care, or physical therapy.
While these methods may help in some cases, they are largely unsuccessful. However, attempts at these non-surgical treatments can serve as documentation and help you qualify for insurance coverage.
Substantial Tissue Must be Removed
Some insurance providers state that a certain amount of breast tissue must be removed to qualify for coverage. Therefore, larger reductions, a G cup to a C cup, for example, have a better chance of coverage. As a general rule, procedures that eliminate at least 500 grams from each breast often qualify.
Permanent Shoulder Grooves
If you suffer from enlarged breasts, you are most likely familiar with indentations in the shoulders from your bra straps. This is a common symptom of macromastia. If you have permanent shoulder grooves in combination with chronic pain, you may be more likely to qualify for insurance coverage.
Contact Us for More Information
When considering breast reduction, it is important to fully understand your insurance coverage. To learn more about how you can maximize your insurance benefits, contact us online or call us at (212) 434-6980.